Urinate After Waking Then Again Within 20 Minutes
Introduction 
Millions of people in the U.s.a. struggle with Overactive Bladder (OAB) symptoms. The most common symptom is the ongoing urgent demand to go to the bathroom. Now.
OAB can interfere with piece of work, going out with friends, exercise and slumber. Information technology can lead y'all to the bath many times during the day or night. Some people leak urine (pee) afterwards this urgent "gotta get" feeling. Others experience afraid they'll leak.
Fortunately, there is assistance and in that location are treatments.
What is OAB and Who Gets It? 
Overactive float is the proper name for a group of bladder symptoms. At that place are three main symptoms:
- A feeling that yous take to get to the bath, urgently.
- Sometimes incontinence, which means that you lot leak urine with the "gotta become" feeling.
- Usually the demand to go to the bath often (often), day and nighttime.
With OAB, yous feel that you need to empty your bladder – even when it's not total. This leads to the feeling that y'all need a bath speedily, right now. You can't control or ignore this feeling. (Although it may feel similar your bladder muscle is squeezing to empty your bladder, in actual fact your bladder muscle may not be squeezing.) If you "gotta go" eight or more than times each mean solar day and night, or fear that urine will leak out before you're ready, you may have OAB.
OAB affects about 33 meg Americans. It'due south not a normal part of crumbling. Information technology's a health trouble that can last for a long time if it's not treated. Many older men (xxx%) and women (40%) struggle with OAB symptoms. Often people don't know nigh treatments that tin help, or they don't enquire for help.
Stress urinary incontinence or SUI is a different float problem. People with SUI leak urine while sneezing, laughing or beingness agile. It is not the same as that sudden "gotta become" feeling from OAB. To acquire more nearly SUI, go to https://www.urologymanagement.org/sui/.
In this guide you volition find clear information well-nigh how to manage OAB. Delight inquire for aid, even if you feel embarrassed. Don't wait, because in that location are several treatments that piece of work well for OAB. Your health care provider should be trained to talk with you lot and aid you manage your symptoms without embarrassment.
For information nigh the other health intendance providers trained to help, click hither.
How the Urinary Tract Works and What Happens with OAB 
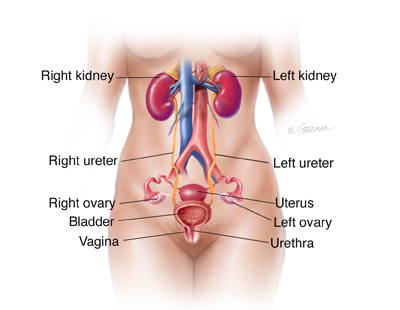
Urinary tract
Medical Illustration Copyright © 2015 Nucleus Medical Media, All rights reserved
The urinary tract is the important organization that removes liquid waste product from our bodies:
- kidneys: two bean-shaped organs that make clean waste matter from the claret and brand urine
- ureters: two sparse tubes that take urine from the kidney to the bladder
- bladder: a balloon-like sac that holds urine until it's time to go to the bathroom
- urethra: the tube that carries urine from the bladder out of the trunk. The urethra has muscles called sphincters that lock in urine. The sphincters open up to release urine when the bladder contracts.
When your bladder is full, your brain signals the bladder. The bladder muscles and then squeeze. This forces the urine out through the urethra. The sphincters in the urethra open and urine flows out. When your float is not full, the bladder is relaxed.
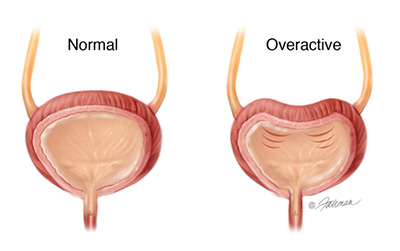
Float and sphincter
Image © 2003 Fairman Studios, LLC
With a healthy bladder, signals in your brain allow y'all know that your bladder is getting full or is full, but you can wait to become to the bathroom. With OAB, yous can't wait. Y'all feel a sudden, urgent demand to go. This can happen even if your bladder isn't total.
Symptoms of OAB 
Urgency: This is the main symptom of OAB. Information technology is a strong (urgent) need to urinate that tin't be ignored. This "gotta get" feeling makes people afraid that they'll leak urine if they don't find a bathroom right away. OAB may as well cause:
- Incontinence (urine leaks): Sometimes OAB causes urine to leak out before getting to the bath. This is called "urgency incontinence." Some people may leak just a few drops, while others can have a sudden gush. (for more data: https://www.urologyhealth.org/urologic-conditions/urinary-incontinence)
- Urinate frequently: OAB may also cause people to go to the bath many times during the day. Experts say that "frequent urination" is when y'all have to go to the bathroom more than than eight (eight) times in 24 hours.
- Wake upward at night to urinate: OAB can wake a person from sleep to get to the bathroom more than in one case a dark. This is chosen "nocturia" by wellness providers.
Some foods and drinks can carp the float. Caffeine, bogus sweeteners, alcohol, chocolate and very spicy foods may make OAB symptoms worse.
OAB does not cause pain. If you feel pain while urinating, you may have an infection. Please talk with your health care provider about pain.
How OAB Can Affect Your Life 
Without treatment, OAB symptoms are uncomfortable. It tin be difficult to get through the day without many visits to the bath. OAB can impact relationships. You lot may not want to practise things you savour considering you worry about finding a bathroom in time. It tin can disrupt your sleep and sex life. It can leave you tired and brusque-tempered, or leaks can lead to a rash or infections. The whole experience tin make anyone feel hopeless and very unhappy.
The good news is that OAB can be controlled. There are treatments available to help.
Finding the Words 
Information technology's normal to feel uncomfortable when talking near OAB symptoms. Who wants to talk about bathroom bug or incontinence?! Even so, knowing more than about OAB is the all-time way to take control of the problem. A little planning will requite you confidence. Here are some tips to help:
- Be prepared: Before your date, gather useful information to help the health care provider learn what's going on. Besides be ready to take notes about what y'all learn. Bring:
- A list of the prescription drugs, over-the-counter medicines, vitamins and/or herbs you take.
- A listing of your past and electric current illnesses or injuries.
- Results from the Think Yous Have Overactive Bladder? Quiz , to aid you discuss your symptoms.
- A pad of newspaper and pen to take notes nigh treatments
- Bring a friend: Ask a close friend or relative to go with y'all to the medico, if y'all don't mind sharing what'due south going on. An "date buddy" can help remind you lot of things y'all may forget to ask, or remind you of things the health care provider said.
- Bring upwards the topic: If your health care provider doesn't inquire about your OAB symptoms, bring up the topic yourself. Don't await until the end of your visit. Make certain you accept time for questions. If a nurse meets with you starting time, tell the nurse about your symptoms.
- Speak freely: Share everything you're experiencing. Your health care provider hears about problems every twenty-four hours. They've heard information technology all! It's OK to tell them nigh your symptoms and how they touch your daily life. Let your health intendance provider know your answers to these questions:
- Do my symptoms brand me terminate doing the things I bask, or forestall me from going to events?
- Am I afraid to be also far away from a bath?
- Have my symptoms changed my relationships with friends or family?
- Practise my symptoms make information technology hard to get a adept night's slumber?
- Enquire questions: A visit to your health care provider is the right time to ask questions. Information technology is best to bring your list of questions with you so you lot don't forget. Nosotros offering some good question to enquire in each section of this guide to help you.
- Follow-up care: Inquire your health intendance provider when you lot should visit over again, and what you should bring with you.
How to Diagnose OAB 
When you tell your health care provider about your symptoms, s/he will inquire more than questions and practise some tests. This is done to diagnose the problem. OR, your provider will tell you the name of a specialist who tin can diagnose and treat yous.
To learn what'south happening, a health intendance provider will likely:
- Ask about your health history: You will be asked about how you experience, how long you lot've had symptoms, and how they touch on you lot. You will be asked about medicine you take (over-the-counter and prescribed). You should likewise talk almost what yous eat and potable during the day. This lets your provider learn about your wellness now and in the past.
- Do a physical exam: Your health intendance provider volition look for things that could cause symptoms. In men and women, they will feel your organs in and below your belly, in your pelvic area. They will besides cheque your rectum.
- Enquire you to keep a "Bladder Diary:" A Float Diary helps you, and your doctor, acquire about daily events and patterns. In this diary you write down how often you go to the bathroom and if/when you leak urine. You tin can use this Float Diary sample to start. You can also download an electronic float diary for your mobile device like The Bladder Pal. This app was developed by AUA Member, Dr. Ronald Yap, through the support of the LeBaron Foundation and the Concord Infirmary Trust.
- Bladder Pal app for Android
- Bladder Pal app for Apple tree
- Do other tests if you lot need them:
- Urine test: a sample of your urine may be tested for infection or blood.
- Bladder browse: This exam shows how much urine is left in your bladder afterward y'all become to the bathroom.
- Cystoscopy: Your health care provider inserts a thin tube with a tiny camera into the float to meet if information technology looks normal or not.
- Urodynamic testing: These tests check to run into how well your lower urinary tract holds and lets-go of urine. One of these tests is call CMG (cystometrogram ).
- Symptom quiz: Many doctors use a written quiz to ask questions about your bladder issues and what causes you the most bother. Accept our OAB Quiz
There are a number of things yous can practise to assistance manage OAB. Anybody has a different feel with what works all-time. You may attempt 1 treatment alone, or several at the same time. You and your wellness care provider should talk about what y'all want from treatment and about each option.
OAB treatments include:
Lifestyle Changes 
To manage OAB, wellness care providers first ask a patient to brand "lifestyle changes". Sometimes these changes are called "behavioral therapy". This could mean that you eat different foods, alter how much, when or what y'all drink, and pre-programme bathroom visits to feel better. Many people find that these changes help. Other people demand to do more.
- Limit food and drinks that bother your bladder: Many people feel better when they alter the way they swallow and beverage. At that place are sure foods known to bother the bladder. You can try taking all of these things out of your diet, then add them back one at a time. Once you learn which foods and drinks make your symptoms worse, you can avoid them. Common foods to avoid:
- Coffee / caffeine
- Tea
- Artificial sweeteners
- Alcohol
- Soda and other fizzy drinks
- Citrus fruit
- Nutrient made with tomatoes
- Chocolate (not white chocolate)
- Spicy foods
- Keep a bladder diary: Writing downward when you make trips to the bathroom for a few days can help you understand your body better. This diary may show you things that make symptoms worse. For instance, are your symptoms worse after eating or drinking a certain kind of nutrient? Are they worse when y'all don't drink enough liquids?
- Double voiding (emptying your bladder twice): This may be helpful for people who have problem fully elimination their bladders. After you become to the bathroom, you await a few seconds and and so try to get over again.
- Delayed voiding: This means that you practice waiting earlier you get to the bathroom, even when you have to go. At first, you lot await just a few minutes. Gradually you may be able to wait two to iii hours at a time. Merely try this if your health care provider tells you to. Some people feel worse or have urine leaks when they expect as well long to go to the bathroom.
- Timed urination: This means that you follow a daily bath schedule. Instead of going when yous feel the urge, you lot go at set times during the day. You lot and your health care provider will create a reasonable schedule. You may try to urinate every two to four hours, whether you lot feel y'all have to become or not. The goal is to preclude that "urgent" feeling and to gain control.
- Exercises to relax your bladder musculus: You may be familiar with exercises to strengthen your pelvic floor muscles, also chosen Kegel exercises. A special exercise using those same pelvic floor muscles may assist relax your bladder during those "gotta go" moments. To do "quick flicks," y'all quickly squeeze and relax your pelvic floor muscles repeatedly. When you feel the urge to go, effort a number of "quick flicks" instead. These exercises tin can assistance control that "gotta go" feeling. It helps to be still, relax and focus on but the exercise. Your health care provider or a physical therapist can assistance yous learn these exercises. Biofeedback may also assist. Biofeedback uses computer graphs and sounds to monitor muscle movement. It tin can aid teach y'all how your pelvic muscles move and how strong they are.
Prescription Drugs 
When lifestyle changes aren't enough, the side by side pace may be to take medicine. Your health care provider tin can tell you almost special drugs for OAB.
There are several types that can relax the bladder muscle. These drugs (for example: Anti-muscarenics and Beta-3 agonists) can help finish your float from squeezing when it'due south not total. Some are taken equally pills, past rima oris. Others are gels or a viscid patch to give you the drug through your peel.
Your wellness care provider volition want to know if the medicine works for you lot. They will check to meet if you go relief or if the drug causes issues, known as "side-effects". Some people get dry oral fissure and dry optics, constipation, or blurred vision.
To help salve symptoms, your wellness care provider may ask you to take different amounts of the drug. Or, give you a different one to effort. Yous may exist asked to make lifestyle changes and accept medicine at the same fourth dimension for better results.
Injections 
If lifestyle changes and medicine aren't working, there are other options. A trained urologist or FPMRS specialist can assist. They may offering bladder injections (shots) of Botox® (botulinum toxin).
Small amounts of Botox® can stop the bladder muscles from squeezing too much. Many tiny injections are used. It gently paralyzes the muscles. Boosted treatments are given when this treatment wears off, anywhere from six to twelve months later. Your doctor will watch how yous're doing to make certain y'all aren't retaining (property in) besides much urine. If urine is not draining well, yous may need to catheterize temporarily.
Nerve Stimulation (Neuromodulation Therapy) 
Another treatment for people who demand extra help is nervus stimulation, also called neuromodulation [pronounced: NER-oh-mahd-yoo-LAY-shun] therapy.
This type of treatment sends electrical pulses to nerves in your bladder. In OAB, the nerve signals betwixt your bladder and brain don't work the right mode. These electrical pulses interrupt the nerve signals, set them right, and improve OAB symptoms.
There are two types:
- Sacral neuromodulation (SNS) changes how the sacral nervus works. This nervus carries signals between the spinal cord and the float. Its job is to help hold and release urine. In OAB, these nerve signals aren't doing what they should. SNS uses a "bladder pacemaker" to control these signals to finish OAB symptoms. SNS is a ii-step surgical process. The first step is to implant an electrical wire under the peel in your lower back. This wire is showtime connected to a handheld "pacemaker" to transport pulses to the sacral nerve. You and your physician will test whether or non this pacemaker can help you. If information technology helps, the 2d step is to implant a permanent pacemaker that can regulate the nervus rhythm.
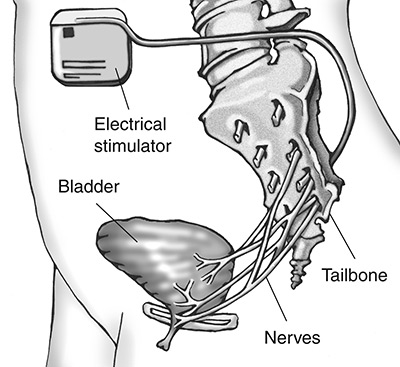
Sacral neuromodulation (SNS)
National Institute of Diabetes and Digestive and Kidney Diseases,
National Institutes of Health - Percutaneous tibial nerve stimulation (PTNS) is another style to correct the nerves in your float. For this type of nerve stimulation you lot will not have to take surgery. PTNS is performed during an role visit that takes virtually 30 minutes. PTNS is washed past placing a small electrode in your lower leg near your ankle. Information technology sends pulses to the tibial nerve. The tibial nerve runs along your knee to the sacral nerves in your lower back. The pulses assistance command the signals that aren't working correct. Often, patients receive 12 treatments, depending on how it'southward working. [This therapy is pronounced: PER-cyoo-TAY-nee-uhs TI-bee-ahl NERV STIM-yoo-LAY-shun.]
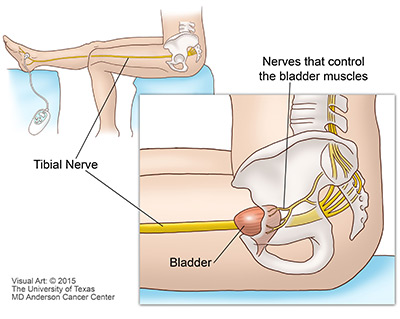
Percutaneous tibial nerve stimulation (PTNS)
(c)2012 The University of Texas Thou.D. Anderson Cancer
Other Resource 
Here are a few more organizations that offering useful data to assist people living with OAB and incontinence.
Urology Care Foundation
1-800-828-7866
The official foundation of the American Urological Clan, the Urology Care Foundation is committed to advancing urologic enquiry and education. Nosotros collaborate with researchers, health care providers, patients and caregivers to improve patients' lives.
American Urological Association
The American Urological Association promotes the highest standards of urological clinical care through pedagogy, research and wellness intendance policy.
Information technology's Time to Talk about OAB
Get the facts. Get diagnosed. Take control.
Club printed materials about OAB, have our "Overactive Bladder Quiz," and download a "Bladder Diary" to track your symptoms.
Information technology's Fourth dimension to Talk about SUI
Notice out more than about Stress Urinary Incontinence, order printed materials and take the SUI quiz.
National Kidney and Urologic Diseases Clearinghouse:
The National Kidney and Urologic Diseases Information Clearinghouse (NKUDIC) is a service of the National Found of Diabetes and Digestive and Kidney Diseases (NIDDK) that provides information on kidney and urologic diseases. The NIDDK is part of the U.Southward. National Institutes of Wellness (NIH).
National Clan for Continence
The National Association for Continence is a national, private, not-profit organization dedicated to improving the quality of life of people with incontinence, voiding dysfunction, and related pelvic floor disorders. NAFC's purpose is to be the leading source for public instruction and advocacy about the causes, prevention, diagnosis, treatments, and management alternatives for incontinence.
Simon Foundation for Continence
The mission of the Simon Foundation is to bring the topic of incontinence out into the open, remove the stigma surrounding incontinence, and provide help and hope to people with incontinence, their families and the wellness professionals who provide their care.
Patient resource provided through the generous support of:

Source: https://www.urologyhealth.org/overactive-bladder
0 Response to "Urinate After Waking Then Again Within 20 Minutes"
Post a Comment